March 31, 2026
What Does Melanoma Look Like?
How to spot it, and what to know so you can get the help you need to stop it.
Looking for Something Else?
“Is This Melanoma?”
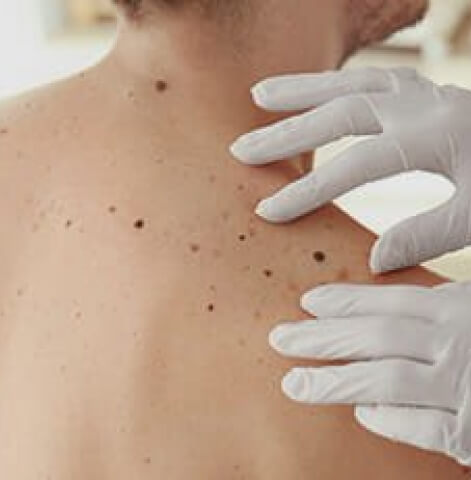
This is one of the most frequently-asked questions we hear. Most cutaneous (skin) melanomas are found by patients, not doctors, so it is important to know your skin and body well so you can recognize when a mole isn’t “just a mole.”
Melanoma can look different from person to person, but if you suspect that a spot on your skin fits the following descriptions, talk to your dermatologist right away. Not all skin cancers and melanomas fall into these categories, so use this list as a starting point:
A Change on the Skin
This could be a new spot, or a change in color, shape or size of a current spot
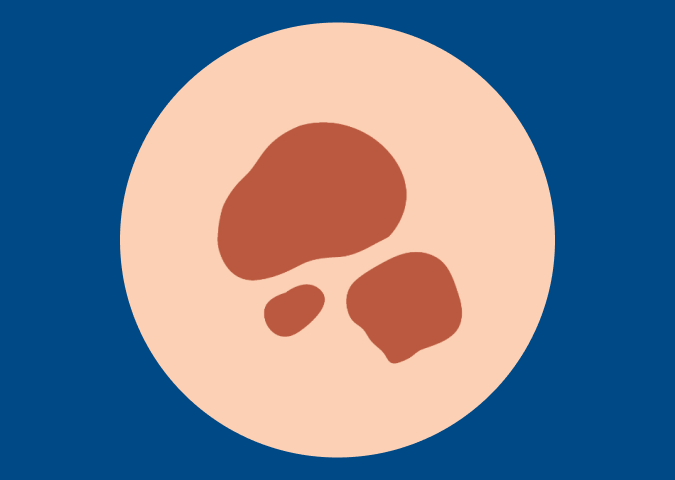
A New Spot, Sore or Mole
If it doesn’t heal or becomes painful and tender
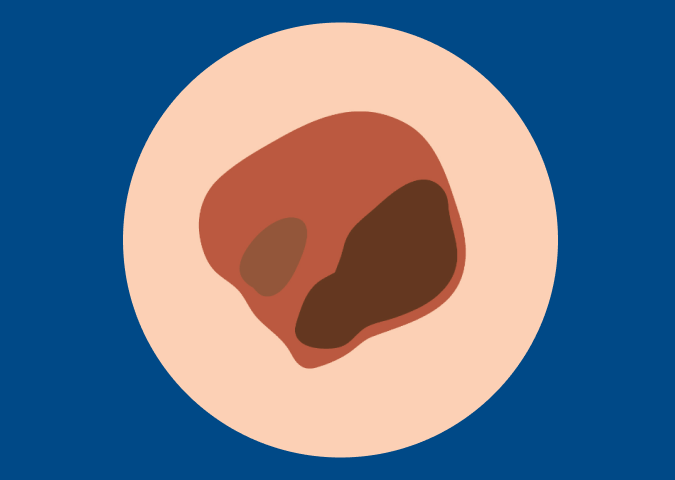
A Mole That is Irritated
Especially take concern if it starts to itch or bleed
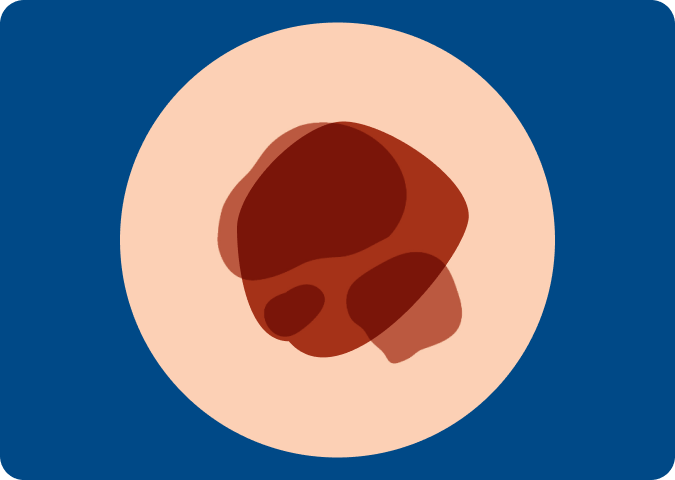
A Firm Red Lump Appears
A firm red lump that bleeds or appears crusty

A Change in in Texture or Look
A spot, sore, mole or lump that looks shiny, waxy, smooth or pale
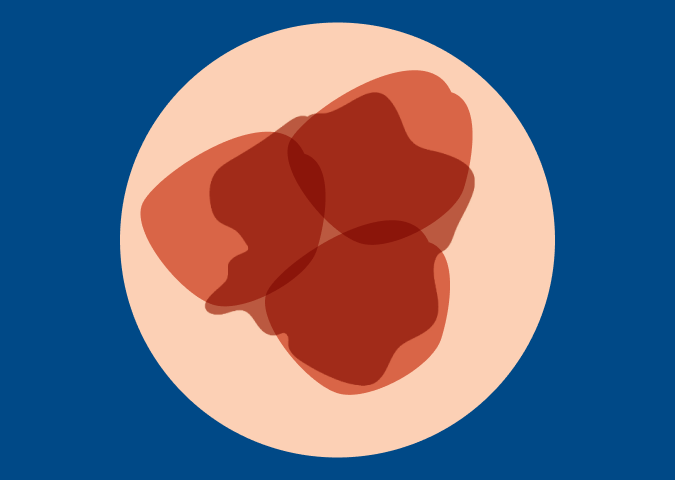
A Dry, Rough Red Spot
A flat, red spot that is rough, dry or scaly
A Dark Spot or Streak
Found under a fingernail or toenail (that hasn’t come from previous trauma to the nail)³
The ABCDEs of Melanoma
These characteristics are used by dermatologists to classify melanomas of the skin. Look for these signs: Asymmetry, irregular Borders, more than one or uneven distribution of Color, or a large (greater than 6mm) Diameter. Finally, pay attention to the Evolution of your moles – know what’s normal for your skin and check it regularly for changes.1-2
Want this information as a handout? We’re proud to offer the ABCDEs in multiple languages:
If you see one or more of these, make an appointment with a dermatologist immediately.
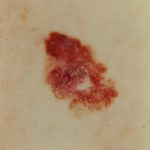
A – Asymmetrical Shape
Melanoma lesions are often irregular, or not symmetrical, in shape. Benign moles are usually symmetrical.
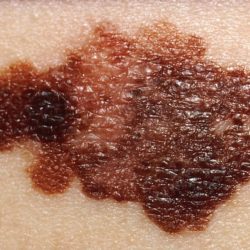
B – Border
Typically, non-cancerous moles have smooth, even borders. Melanoma lesions usually have irregular borders that are difficult to define.
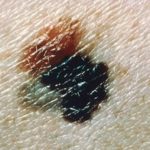
C – Color
The presence of more than one color (blue, black, brown, tan, etc.) or the uneven distribution of color can sometimes be a warning sign of melanoma. Benign moles are usually a single shade of brown or tan.
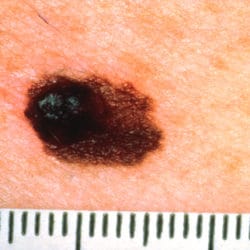
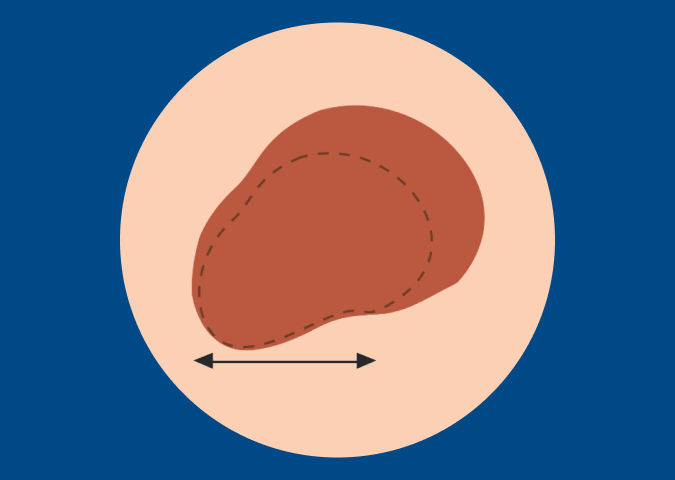
D – Diameter
Melanoma lesions are often greater than 6 millimeters in diameter (approximately the size of a pencil eraser).
E – Evolution (or change)
The evolution of your mole(s) has become the most important factor to consider when it comes to diagnosing a melanoma. Knowing what is normal for YOU could save your life. If a mole has gone through recent changes in color and/or size, bring it to the attention of a dermatologist immediately.
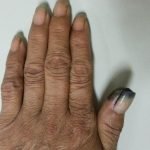
Acral Melanoma Pictures.
Under the nail bed, this is often referred to as subungual melanoma.
Source: Photos courtesy of Dr. Guowen Wang in the Department of Soft Tissue Cancer, Tianjin Cancer Center, Tianjin Medical University

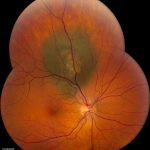
Ocular Melanoma Pictures.
Medium choroidal melanoma near the optic disc showing blood where the tumor has ruptured through the overlying Bruch’s membrane to form a “collar button”; Source: Photos courtesy of Dr. J. William Harbour of Bascom Palmer Eye Institute
Have questions about ocular melanoma? Read about CURE OM, the MRF’s initiative for ocular melanoma.
Exploring Types of Melanoma
Events

Jul 30, 2026 ET
Ask the Expert: The Evolving Role of ctDNA in Melanoma Treatment and Surveillance




Patient Resources
The MRF is committed to providing the most up-to-date education and support resources for melanoma patients and their loved ones.
Citations
Content last updated: June 1, 2021
National Cancer Institute, Division of Cancer Epidemiology and Genetics
Centers for Disease Control and Prevention
National Cancer Institute, Division of Cancer Epidemiology and Genetics, https://moles-melanoma-tool.cancer.gov/